|
CASE REPORT |
https://doi.org/10.5005/jp-journals-10080-1543
|
Chronic Isolated Dorsal Dislocation of the Lunate. A Rare Presentation of Carpal Instability
1,3–6Department of Orthopedic Surgery, Hospital 12 de Octubre, Madrid, Spain
2Hospital Universitario Fundacion Jimenez Diaz, Madrid, Spain
Corresponding Author: Diego Alonso-Tejero, Department of Orthopedic Surgery, Hospital 12 de Octubre, Madrid, Spain, e-mail: diegoal1228@gmail.com
How to cite this article: Alonso-Tejero D, Luengo-Alonso G, Jiménez-Díaz V, et al. Chronic Isolated Dorsal Dislocation of the Lunate. A Rare Presentation of Carpal Instability. Strategies Trauma Limb Reconstr 2022;17(1):59–62.
Source of support: Nil
Conflict of interest: None
ABSTRACT
Isolated dorsal lunate dislocation is a rare injury. Only one case has been reported previously in which the treatment was performed in the chronic stage. In this report, we present the case of a 49-year-old handworker male who presented a dorsal dislocation of the lunate after a traffic accident. He was referred to our clinic 2.5 months later due to an initial misdiagnosis. Surgical treatment was performed and consisted of an open reduction using a nerve-sparing dorsal approach. A complete rupture of the perilunate ligaments and a marked instability of the lunate were detected. Stabilisation of the scapholunate, lunotriquetral and scaphocapitate spaces with a compression screw and Kirschner wires, respectively, was performed. The persistence of pain and functional limitation after the surgery along with an insufficient reduction of the scapholunate space on the X-ray and the development of a fistula on the ulnar edge of the carpus prompted reintervention. A hardware-free total wrist arthrodesis was preferred over other procedures, such as proximal row carpectomy, owing to the important articular damage. At the 3-month follow-up, he was clinically stable, consolidation of arthrodesis was documented and he had returned to his previous activities. Isolated dorsal dislocation of the lunate is a rare lesion. There is no consensus on the management of isolated chronic dislocations of the lunate. The frequent delay in the diagnosis compromises the final outcome of reconstructive techniques and introduces the risk of residual instability, increasing the incidence of chronic pain associated with post-traumatic osteoarthritis. In the case of chronic lesions, treatment with palliative techniques, such as proximal carpectomy or joint arthrodesis, should be considered.
Keywords: Arthrodesis, Chronic, Dislocation, Dorsal, Lunate.
INTRODUCTION
Carpal dislocations are very uncommon injuries that generally result from high-energy trauma. The carpus can be viewed as a complex of bones joined together by an intricate set of intrinsic and extrinsic ligaments, allowing both motion and strength transmission. Lunate dislocation often occurs in the volar direction as the final stage of the perilunar injury described by Mayfield et al.1 In this setting, disruptions of scapholunate and lunotriquetral ligaments, the space of Poirier and dorsal radiolunate capsule occur in a predictable sequence.
An isolated dorsal dislocation of the lunate is an exceptionally rare lesion with very few reports in the literature, and with only one in which the treatment was performed at the chronic stage. A major challenge in the management of carpal dislocations is early identification and treatment. Up to 25% of injuries remain undiagnosed 6 weeks after the initial injury.2 This strongly influences the final outcome and, in some cases, determines the therapeutic approach.
In this case report, we present an unrecognised isolated dorsal dislocation of the lunate diagnosed 10 weeks after a motor vehicle accident. The treatment and outcome are described as high risk of complications, such as persistent instability, chronic pain and reduced range of motion, all of which are related to the failure to address this injury in the acute period.
CASE DESCRIPTION
A 49-year-old, right-handed heavy manual worker male sustained an injury to his left wrist following a motor vehicle accident. He attended his general practitioner initially with a swollen and painful left wrist. A complete radiographic evaluation was performed and interpreted as normal by both his physician and a radiology specialist despite the images showing a dorsal lunate dislocation (Fig. 1).
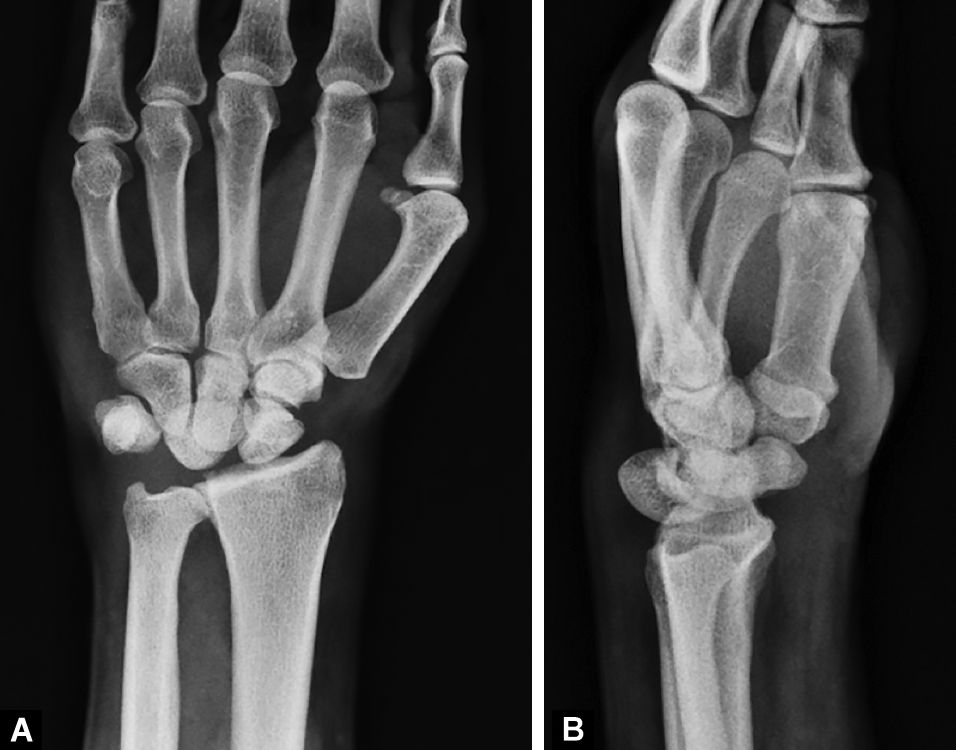
Fig. 1A and B: Initial plain radiographs of the wrist (anteroposterior and lateral views) show a dorsal dislocation of the lunate with corresponding distortion of the Gilula’s lines. There is no evidence of any carpal bone fracture
An open reduction was performed through a nerve-sparing dorsal capsulotomy.3 The lunate was identified in the subcutaneous tissue with minor residual ligament attachments. A complete rupture of scapholunate and lunotriquetral ligaments was noted with no remnants to facilitate a primary repair (Fig. 2). There was no evidence of articular cartilage disruption of the lunate or the proximal pole of the capitate. Although the lunate could be reduced into its place gently, this was very unstable and dislocated again with the wrist in the neutral position. A K-wire was used as a joystick and worked to hold the lunate in its place temporarily. We placed a 24-mm headless cannulated screw between the scaphoid and lunate. Additionally, we used K-wires connecting triquetrum to lunate and scaphoid to capitate (Fig. 3). An implant-related fracture occurred in the scaphoid intraoperatively.

Fig. 2: Intraoperative picture of the open reduction. Intraoperative picture shows the dorsal capsule retracted and the lunate dislocated with no soft tissue remnants. Intercarpal ligament deterioration prevented direct repair
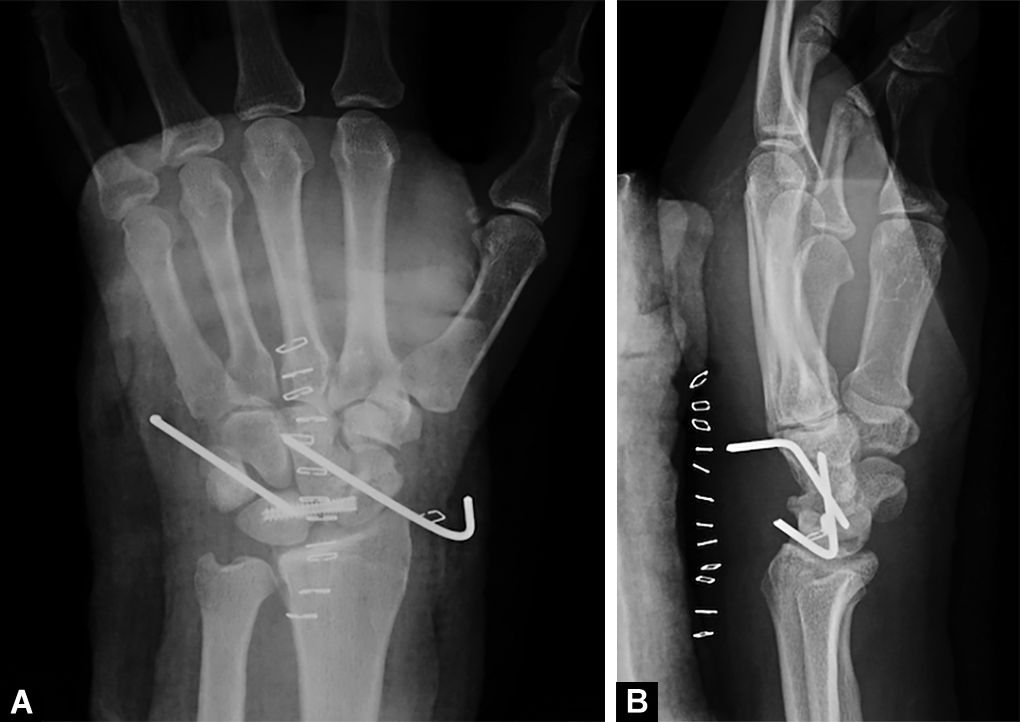
Fig. 3A and B: Postoperative plain radiographs (anteroposterior and lateral views) show a correct articular reduction. A cannulated headless screw was placed between scaphoid and lunate. K-wires connecting lunate to triquetrum and scaphoid to capitate contributed to additional stability
After surgery, the wrist was immobilised with a splint below the elbow for 6 weeks. By that time, the K-wires were removed and active non-weight-bearing range of motion exercises were encouraged. Two months after surgery, the patient reported pain with daily activities and severe stiffness. Radiologically, the lunate appeared dorsally luxated and a decrease in carpal height was observed (Fig. 4).
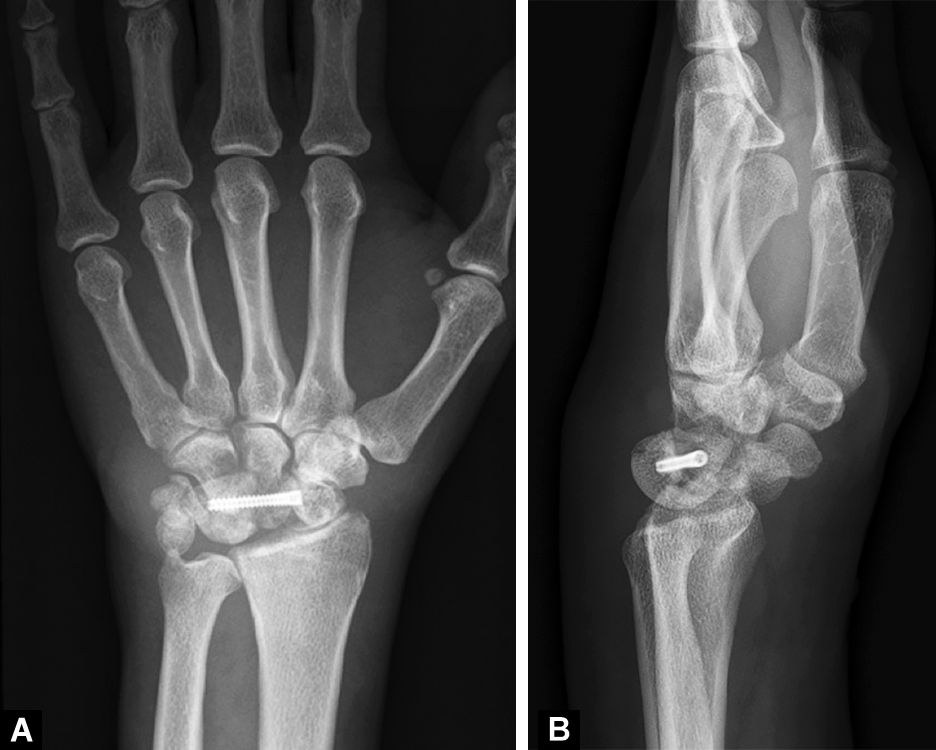
Fig. 4A and B: Postoperative radiographs at 2 months show a relapse of the instability. The lunate is dorsally dislocated and a decrease in carpal height can be observed
A hardware-free wrist arthrodesis was chosen because of the appearance of a fistula where the ulnar side K-wire was placed previously. Although oral antibiotic treatment was prescribed, an infection could not be ruled out prior to the revision surgery. Nine months after the initial injury, a radiocarpal fusion was performed. Generalised osteoarthritis of the radiocarpal joint was observed. The fixation was performed with two K-wires in a cross configuration. Cancellous bone autograft from the distal dorsal radius and biphasic calcium phosphate composite block bone graft were incorporated at the fusion site.
Surgical wound infection occurred in the post-operative period that was treated with oral antibiotics, local debridement and dressings containing silver. Twenty-four months after surgery, the patient does not report any further pain or tenderness. He has resumed his work fully as a construction worker. He does not refer to disability. Functional assessment using the QuickDASH questionnaire was excellent, with a score of 11 points. Radiographic evaluation shows a successful radiocarpal arthrodesis (Fig. 5).

Fig. 5A and B: Postoperative radiographs 24 months after wrist arthrodesis show a successful radiocarpal arthrodesis. The patient remains asymptomatic with excellent function
DISCUSSION
Isolated dorsal dislocation of the lunate is a very rare injury with few cases described in the literature. This case is the second example of a chronic isolated dorsal dislocation of the lunate. The first was reported by Seidenstein et al.4 A dorsal dislocation of the lunate after wrist hyperflexion was diagnosed correctly only after 3 months from the initial injury. A lunate excision was performed as definitive treatment. Almost complete wrist motion and strength were restored with only mild residual pain.
Some cases of isolated dorsal lunate dislocations have been described in which definitive treatment could be performed in an acute or subacute phase. The case described by Bilos et al.5 was of a dorsal lunate dislocation after a repetitive low-energy trauma. An open reduction and direct repair of the affected ligaments were achieved. Siddiqui et al.6 reported a case caused by a low-energy trauma where a Kirschner wire, used as in the Kapandji technique, was enough for keeping the lunate in its place. Both cases reported excellent functional outcomes. Finally, Zaidenberg et al.7 communicated a dorsal lunate dislocation after a fall on a dorsally flexed wrist. An anatomical reduction and a ligament repair using suture anchors were performed. The clinical and functional outcome could not be evaluated because of a foreign body reaction to the suture anchors which caused severe chondral damage to the lunate and scaphoid. Other cases of dorsal lunate dislocation reported in the literature have presented with associated lesions, such as carpal bone fractures or tendon injuries.
The most accepted theory for perilunate dislocations was proposed by Mayfield et al.1 He postulated that the injury occurred after a force applied to the wrist in extension, ulnar deviation and intercarpal supination. A predictable pattern of injury develops starting from the radial to the ulnar side and follows four consecutive stages. In the fourth stage, dorsal radiocarpal ligament disruption allows the lunate to dislocate anteriorly as the rest of the carpus returns to the neutral position. Additionally, a reverse mechanism was described by Viegas et al.,8 in which the injury advances from the ulnar to the radial side when the wrist is placed in extension and intercarpal pronation. This pattern causes a volar intercalated segment instability lesion. It is proposed by some authors that the isolated dislocation of the lunate might be caused by a mechanism contrary to the volar dislocation as a final step of the pattern described by Viegas.
The true mechanism of injury involved in an isolated dorsal lunate dislocation is unknown. Neither the theory described by Mayfield nor the one by Viegas describes a scenario in which an isolated dorsal lunate dislocation is present. Despite the few cases of this kind of lesion reported in the literature, a wide variety of injury mechanisms have been described. Most authors agree on high-energy trauma occurring on a hyperflexed wrist. However, Zaidenberg et al.7 reported a fall onto an outstretched and dorsally flexed wrist, and Siddiqui et al.6 described a low-energy mechanism. In this case, the position of the wrist at the moment of impact is unknown.
Historically, the management of carpal instability is the closed treatment for acute perilunate dislocations. The trend today has changed; early open anatomic reduction, internal fixation and ligament repair are considered a gold standard by most authors.9–11 The open approach allows the surgeon to assess the condition of the articular cartilage directly and to choose between a direct repair or a non-reconstructive procedure. Nonetheless, despite early and appropriate treatment, complications, such as pain, stiffness and loss of strength are common and this ranges from 20 to 30% of the cases.11,12 In the last few years, some authors have shown encouraging results with an arthroscopically assisted surgery without direct ligament repair in terms of carpal stability, wrist motion and functional scores.13
According to Herzberg’s classification, chronic dislocation is that which persists unreduced for more than 45 days. Up to 25–26% of the perilunate dislocations are missed initially. A delay in treatment is related to a worse functional and radiological outcome.2 Complications, such as chronic carpal instability, avascular necrosis, reduced mobility and arthritis are associated with carpal dislocations not treated at an early stage.14
Adequate results for the treatment of chronic perilunate lesions can be achieved with an open reduction and internal fixation procedure.15–18 Ligament reconstruction is usually not possible due to tissue distortion and extensive scarring. When persistent instability is observed, ligamentoplasty techniques, such as that described by Corella et al.,19 are indicated if correct reduction can be achieved in the absence of chondral damage. There is no generally accepted consensus on the upper time limit by which open reduction can be performed for these injuries which have been missed. Siegert et al.20 achieved satisfactory results in unrecognised cases that were present for up to 35 weeks.
Insufficient accuracy in reduction and the presence of articular damage are also predictors of a poor outcome.11,16,17 Salvage procedures, such as partial or complete wrist arthrodesis, should be considered in cases where a satisfactory reduction is not obtained or when serious articular damage is present. Proximal row carpectomy is an alternative for cases where the articular surfaces of the proximal pole of the capitate and the lunate fossa of the radius are intact. Interventions, such as partial or complete lunate excision, have been abandoned due to unfavourable results.20 An arthroscopically assisted technique has been described for the management of chronic injuries, the results of which are yet to be reported.21
A satisfactory reduction could not be achieved in this case due to technical events during the surgery. The lunate soon re-dislocated to its dorsal position after removing the K-wires. Persistent carpal instability together with local infection made it mandatory to consider a salvage procedure. A proximal row carpectomy was not an option in this case as important articular damage was identified intraoperatively at the proximal pole of the capitate. A radiocarpal arthrodesis was chosen as the preferred treatment. A hardware-free technique was favoured in order to minimise the risk of a new surgical infection.
In conclusion, the quality of the reduction and the level of destruction of the cartilage of the carpal bones are important factors as well as the time elapsed since the initial injury, in determining a management strategy in chronic dorsal lunate dislocation. Given the experience of this case, we recommend salvage procedures, such as partial or complete wrist arthrodesis or proximal row carpectomy, in the treatment of this pathology.
ORCID
Diego Alonso-Tejero https://orcid.org/0000-0002-6071-5062
Gonzalo Luengo-Alonso https://orcid.org/0000-0003-3516-5043
Lorena García-Lamas https://orcid.org/0000-0001-8370-8327
David Cecilia-López https://orcid.org/0000-0002-3455-9561
REFERENCES
1. Mayfield JK, Johnson RP, Kilcoyne RK. Carpal dislocations: Pathomechanics and progressive perilunar instability. J Hand Surg 1980;5(3):226–241. DOI: 10.1016/S0363-5023(80)80007-4
2. Herzberg G, Comtet JJ, Linscheid RL, et al. Perilunate dislocations and fracture-dislocations: a multicenter study. J Hand Surg 1993;18(5):768–779. Available from: http://www.ncbi.nlm.nih.gov/pubmed/8228045.
3. Hagert E, Ferreres À, Garcia-Elias M. Nerve-sparing dorsal and volar approaches to the radiocarpal joint. J Hand Surg 2010;35(7):1070–1074. DOI: 10.1016/j.jhsa.2010.03.032.
4. Seidenstein H. Two unusual dislocations at the wrist. J Bone Joint Surg Am 1956;38A(5):1137–1141. Available from: http://www.ncbi.nlm.nih.gov/pubmed/13367090.
5. Bilos ZJ, Hui PW. Dorsal dislocation of the lunate with carpal collapse. Report of two cases. J Bone Joint Surg Am 1981;63(9):1484–1486. Available from: http://www.ncbi.nlm.nih.gov/pubmed/7320040.
6. Siddiqui N, Sarkar S. Isolated dorsal dislocation of the lunate. Open Orthop J 2012;6(1):531–534. Available from: http://www.ncbi.nlm.nih.gov/pubmed/23248723.
7. Zaidenberg EE, Roitman P, Gallucci GL, et al. Foreign-body reaction and osteolysis in dorsal lunate dislocation repair with bioabsorbable suture anchor. Hand 2016;11(3):368–371. DOI: 10.1177/1558944715627632.
8. Viegas SF, Patterson RM, Peterson PD, et al. Ulnar-sided perilunate instability: an anatomic and biomechanic study. J Hand Surg 1990;15(2):268–278. DOI: 10.1016/0363-5023(90)90107-3.
9. Vitale MA, Seetharaman M, Ruchelsman DE. Perilunate dislocations. J Hand Surg 2015;40(2):358–362. DOI: 10.1016/j.jhsa.2014.10.006.
10. Krief E, Appy-Fedida B, Rotari V, et al. Results of perilunate dislocations and perilunate fracture dislocations with a minimum 15-year follow-up. J Hand Surgery 2015;40(11):2191–2197. DOI: 10.1016/j.jhsa.2015.07.016.
11. Israel D, Delclaux S, André A, et al. Peri-lunate dislocation and fracture-dislocation of the wrist: Retrospective evaluation of 65 cases. Orthop Traumatol Surg Res 2016;102(3):351–355. DOI: 10.1016/j.otsr.2016.01.004.
12. Kremer T, Wendt M, Riedel K, et al. Open reduction for perilunate injuries-clinical outcome and patient satisfaction. J Hand Surg 2010;35(10):1599–1606. DOI: 10.1016/j.jhsa.2010.06.021.
13. Oh WT, Choi YR, Kang HJ, et al. Comparative outcome analysis of arthroscopic-assisted versus open reduction and fixation of trans-scaphoid perilunate fracture dislocations. Arthroscopy 2017;33(1):92–100. DOI: 10.1016/j.arthro.2016.07.018.
14. Wilke B, Kakar S. Delayed avascular necrosis and fragmentation of the lunate following perilunate dislocation. Orthopedics 2015;38(6):e539–e542. Available from: http://www.ncbi.nlm.nih.gov/pubmed/26091230.
15. Komurcu M, Kürklü M, Ozturan KE, et al. Early and delayed treatment of dorsal transscaphoid perilunate fracture-dislocations. J Orthop Trauma 2008;22(8):535–540. DOI: 10.1097/BOT.0b013e318183eb23.
16. Kailu L, Zhou X, Fuguo H. Chronic perilunate dislocations treated with open reduction and internal fixation: results of medium-term follow-up. Int Orthop 2010;34(8):1315–1320. DOI: 10.1007/s00264-009-0926-7.
17. Dhillon MS, Prabhakar S, Bali K, et al. Functional outcome of neglected perilunate dislocations treated with open reduction and internal fixation. Indian J Orthop 2011;45(5):427–431. DOI: 10.4103/0019-5413.83138.
18. Massoud AHA, Naam NH. Functional outcome of open reduction of chronic perilunate injuries. J Hand Surg 2012;37(9):1852–1860. DOI: 10.1016/j.jhsa.2012.06.009.
19. Corella F, Ocampos M, Laredo R, et al. Arthroscopic “S”-shaped ligamentoplasty for floating lunate. Tech Hand Upper Extrem Surg 2020;24(4):194–206. DOI: 10.1097/BTH.0000000000000291.
20. Siegert JJ, Frassica FJ, Amadio PC. Treatment of chronic perilunate dislocations. J Hand Surg 1988;13(2):206–212. DOI: 10.1016/S0363-5023(88)80049-2.
21. Bhatia DN. Arthroscopic reduction and stabilization of chronic perilunate wrist dislocations. Arthroscopy Tech 2016;5(2):e281–e290. DOI: 10.1016/j.eats.2015.12.008.
________________________
© Jaypee Brothers Medical Publishers. 2022 Open Access This article is distributed under the terms of the Creative Commons Attribution-Non Commercial-share alike license (https://creativecommons.org/licenses/by-nc-sa/4.0/) which permits unrestricted distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. If you remix, transform, or build upon the material, you must distribute your contributions under the same license as original. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.